
Blog
-
Experience cataract surgery step by step
Practical example – Cataract surgery on Mrs. H. (55 years old)
Date of surgery: Monday, February 22, 2021
Situation before the procedure
- Visibility: only shadows visible at 3 meters distance
- Diagnosis: very dense cataract, which severely limited daily functioning
Course of the surgery
- The natural cloudy lens was removed through a micro-incision of only 2 mm
- A foldable implant lens was carefully injected
- The artificial lens unfolded by itself and fell into place perfectly in the lens capsule
- The positioning was optimal and the procedure went smoothly
After a few minutes
- The eye structures were stable
- The clarity of the artificial lens was immediately visible
- The patient was able to perceive light and contours better shortly after the operation
🌟 This example illustrates how even in advanced cataracts, safe, precise and effective intervention is possible with modern microsurgery.
Would you like to know whether cataract surgery is also a solution for you?
📅 Make an appointment for a consultation.Before the procedure: Dense cataract
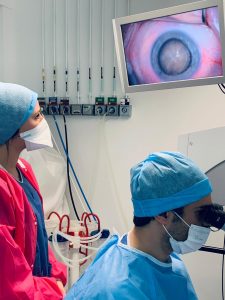
Insertion of the folded implant lens through a 2 mm micro-incision
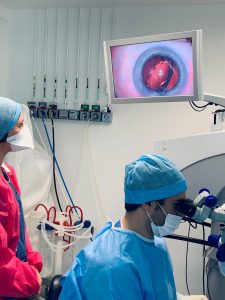
Good positioning of the implant lens
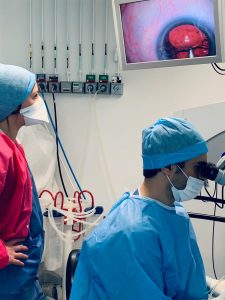
Image a few minutes after the procedure
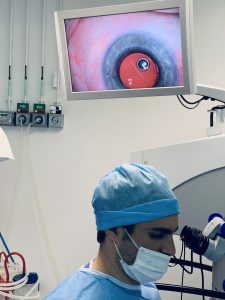
-
Strabismus (Squinting)
Strabismus, also called “lazy eye” or “wandering eye,” is a condition in which one or both eyes can deviate inward, outward, upward, or downward.
In children over six months of age, a fluctuating strabismus can occur. This can be normal in some cases, but it is important to have an ophthalmological examination to rule out any underlying problems.
Some children are born with strabismus, while in others it may be the result of an imbalance in the eye muscles.
Signs and symptoms of strabismus include a child who looks cross-eyed, has difficulty judging distances and picking up objects, squinting one eye to see better, or experiences dizziness.
Early diagnosis of the underlying cause is essential to prevent permanent vision loss. Treatment for strabismus can be done in several ways: by covering the stronger eye to stimulate the weaker eye, wearing glasses, using eye drops, eye muscle exercises or surgery to correct the position of the eyes.
-
Presbyopia
Presbyopia is a naturally evolving process where it becomes increasingly difficult to see clearly up close as one ages.
Suddenly, reading a newspaper or a menu becomes difficult unless one holds it at arm's length — often with great difficulty and visual fatigue as a result.
The eye lens, the so-called crystalline, functions as a natural lens that makes it possible to focus and project images onto the retina. However, from the age of about 40, this lens gradually loses its suppleness and flexibility. It can no longer bulge sufficiently to focus properly on nearby objects.
The result is that the eye no longer sees nearby objects sharply and clearly. The images become blurred, because the focus falls behind the retina. This leads to increasing difficulties in seeing up close.
-
Astigmatism
A person with astigmatism sees objects distorted because the light rays are only partially focused on the retina. Only part of the image is projected onto the retina. Astigmatism can occur on its own or in combination with nearsightedness (myopia) or farsightedness (hyperopia).
Astigmatism can be corrected by flattening the cornea on the most curved side and/or curving the flattest side, so that the cornea becomes perfectly round.
This condition can start in childhood or develop later in life. A simple correction is possible if it is the cause of vision problems. Some signs and symptoms of astigmatism can include headaches, eyestrain, difficulty reading, and general fatigue.
Depending on the severity, glasses or contact lenses may be needed. Refractive surgery with a laser can correct astigmatism up to 5 diopters.
-
Farsightedness (Hyperopia)
Farsightedness is often characterized by an eye that is too “short”. Vision is blurrier up close than at a distance.
It is often present from an early age and can sometimes correct spontaneously as the child grows.
If it persists into adulthood, the hyperopia can be corrected by making the cornea more curved using laser treatment.
Hyperopia can be corrected with glasses, contact lenses, or refractive surgery, which shifts the projection of the image onto the retina so that vision becomes sharp.
There are several signs and symptoms including: permanent strabismus or only when the child is tired, leading to rubbing the eyes, lack of interest in school with a crooked posture when writing, the child holds books too close to the face leading to nausea after reading.
-
Chalazion: blockage of a sebaceous gland in the eyelid
A chalazion is caused by an inflammation resulting from a blockage of the duct of a meibomian gland, located in the upper and/or lower eyelid.
This manifests as a small lump in the eyelid, which may increase in size over the course of a few days. The swelling may become red, tender or painful, and may sometimes be accompanied by a warm feeling around the eyelid.

Natural course and infectiousness
In most cases, a chalazion will disappear spontaneously within a few weeks without any medical consequences. A chalazion is not contagious.
Chalazion or stye (organlet)?
Although both a chalazion and a stye present as a lump in the eyelid, they are two different conditions:
- An orgelet is an acute infection of a sebaceous gland and is usually painful and inflamed.
- A chalazion, on the other hand, is not an infection, but a sterile inflammatory response of the body to accumulated sebum.
With a chalazion, the oil in the meibomian gland becomes too thick to drain normally. This causes it to build up and cause swelling. Sometimes the gland wall breaks, causing the oil to spill into the surrounding tissue. This leads to an inflammatory response, which can result in scarring.
Treatment of a chalazion
Treatment is usually simple and may include:
- Warm compresses: 5 to 10 minutes, four times a day, to reduce swelling and help the gland drain.
- Antibiotic eye drops or ointment: if there are signs of an associated bacterial infection.
- Cortisone injection: In rare cases, an anti-inflammatory drug may be injected directly into the chalazion to reduce swelling.
- Surgical removal: if the chalazion persistent, causes discomfort or for cosmetic reasons.
In case of recurring or multiple chalazions
In frequent or multiple chalazions, consideration should be given to a general sebaceous gland disorder, such as acne rosacea. In this case, long-term treatment with oral medication may help to improve the composition of the sebum and prevent new blockages.
-
Amblyopia (Lazy eye)
Amblyopia is characterized by decreased vision in an anatomically healthy eye that fails to send correct visual signals to the brain.
This is because the eye and brain do not work well together during early development. The eye is, as it were, “switched off” by the brain, which prefers the other, better-seeing eye.
Amblyopia is preventable or correctable in most cases, provided the underlying cause is treated before the age of six. Early detection and treatment are therefore essential for good visual development.
-
Obtain a duplicate of a prescription or invoice
Send us an email to manager@vision-centrum.be so that we can identify you properly and make the necessary preparations.
You must provide your exact contact details as well as the date and time of your appointment.
The practice is open daily from 9:00 AM to 6:00 PM, except on Thursdays (until 2:00 PM) and Fridays (until 4:30 PM).
-
Following cataract surgery
You will be discharged from the hospital the same day. You will wear an eye bandage and a protective cap to prevent eye injuries. These can be removed after a few hours.
Visual acuity returns to normal a few days after surgery, but this depends on the patient and the severity of the cataract. The more advanced the cataract, the longer the recovery may take.
A treatment is prescribed for 6 weeks, consisting of an antibiotic drop and an anti-inflammatory to prevent possible inflammation.
There may be some symptoms after the operation, but these are not alarming:
- The eyes may be red and feel gritty. This is normal and is due to healing, it may take a few days.
- Blurred vision on the day of surgery and the following day is normal.
- Double vision may occur due to the anesthesia, but this is short-lived.
You can resume your daily activities without problems, but be careful with sports. The eye remains fragile, even when the vision is clear again. For sports that cause shocks, it is recommended to wait 3 weeks. You can wash your hair, but avoid contact of the eye with water. You can keep your old glasses or replace them with glasses with neutral lenses if they cause discomfort.